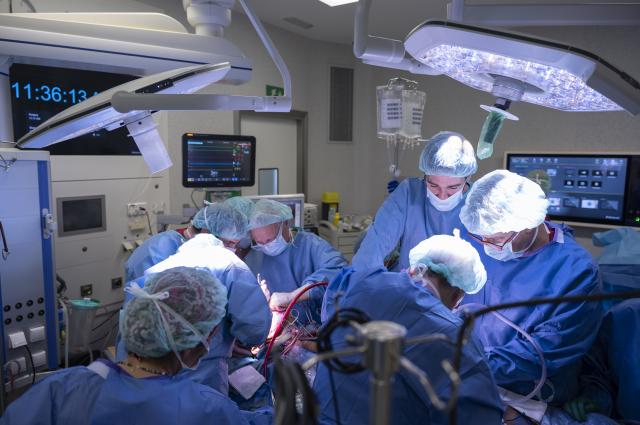
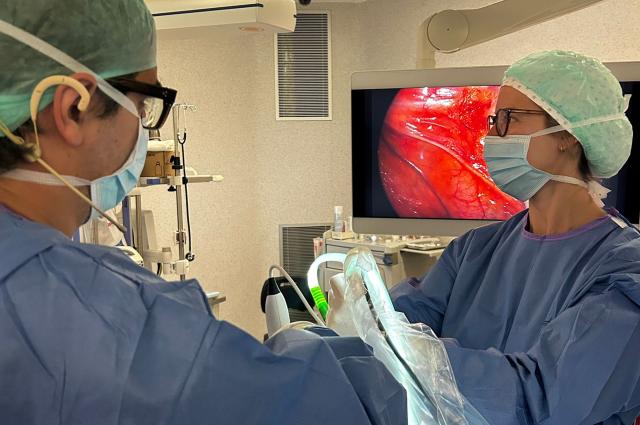
The goal of the Intensive Medicine Department is the diagnosis and treatment of critical patients. It also promotes and designs highly complex, innovative programmes, such as extracorporeal cardiopulmonary support (veno-venous ECPS) or the post-operative care of transplant patients.
The Department is involved in research and education at graduate, post-graduate and ongoing training level. It consists of three units: one dealing in care for patients recovering from Heart Surgery and two multi-purpose units.
All its activities are aimed at meeting the healthcare needs and expectations of the population, with criteria of equity, maximum efficiency and quality, thanks to the active commitment of its entire team of professionals.
Main Building at Bellvitge University Hospital
c/ Feixa Llarga, sn. | 08907 L’Hospitalet de Llobregat. Barcelona
Floor 1, 2 and 3 | Telephone number 93 260 76 46

 Presentation
Presentation Staff
Staff Relevant aspects
Relevant aspects Location
Location News
News